BY: AMELIA CHEN
I have a lot of fears, some more logical than others. And I’d probably count a meat allergy among the more logical ones. I first learned about this almost-unbelievable red meat allergy in a Radiolab podcast, where guest Amy Pearl shared her story about how she discovered she could no longer eat red meat [3]. I know, I thought it sounded absurd, too.
Amy Pearl was tipped off to the existence of this allergy after she began experiencing typical allergic reactions, such as gastrointestinal symptoms and hives, in association with red meat consumption. However, the catch was that at the time, a meat allergy was fairly unheard of. It wasn’t until other patients began experiencing anaphylactic shock in response to the cancer drug, cetuximab, that the culprit of these allergy symptoms was identified as galactose-alpha-1,3-galactose, or alpha-gal [1]. It just so happens that alpha-gal is the sugar present in cetuximab, as well as in all non primate mammals. Following this, allergy researcher Thomas Platts-Mills had noted the link between the drug and high levels of alpha-gal antibodies in cetuximab sensitive individuals. And since alpha-gal is also ubiquitous in cattle, pigs, and lambs, Pearl’s suspicions were confirmed. Unlike most allergies, including that to cetuximab, symptoms are delayed at least two hours and can even take as long as five hours to develop after eating red meat, making this a difficult allergy to diagnose [5]. People don’t usually consider the thing they ate hours before feeling discomfort.
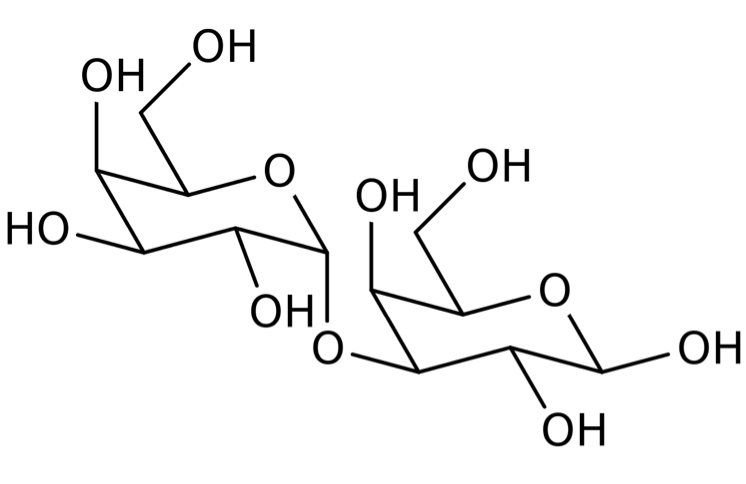
https://en.wikipedia.org/wiki/Galactose-alpha-1,3-galactose
So how does someone who has enjoyed meat, such as a hearty sized steak or rack of ribs their entire lives, suddenly develop an allergy to it? Cases of cetuximab and red meat hypersensitivity were primarily being reported in the southeastern United States, where Rocky Mountain Spotted Fever, a tick-transmitted disease, was also common. So in the name of science, Platts-Mills decided to conduct his own investigation of a possible link between tick bites and the red meat allergy… by going for a hike. And getting bitten by ticks. Sure enough, Platts-Mills contracted the alpha-gal allergy, and the level of alpha-gal antibodies in his blood was also higher [2].

https://www.muscleforlife.com/is-red-meat-bad-for-you/
Red meat allergies as a result of tick bites have affected several thousand people in the US alone, and I can’t imagine many of them are happy about it. However, there is a silver lining to this situation, with meat alternatives being a growing trend in the food industry, there may be hope for all the red-meat-allergic-meat lovers out there. The hope I’m referring to is largely surrounded on the idea of cultured meat. You would think that the ability to build food from the ground up lends itself to customization – put in what we want and take out what we don’t. However, forming a hamburger patty for someone who breaks out in hives after eating red meat is not as easy as just leaving out the alpha-gal stock solution. Humans and primates lack alpha-gal because they also lack the enzyme that adds this sugar to cell surfaces – alpha-1,3-galactosyltransferase [4]. Therefore, to rid meat of alpha-gal, we must also inactivate the enzyme, and there just so happens to be a company that has done that in pigs. Revivicor has knocked out the enzyme in order to increase the success rate of transplanted tissues and organs in humans, and this technology could conceivably be applied to the development of alpha-gal-free red meat down the line.
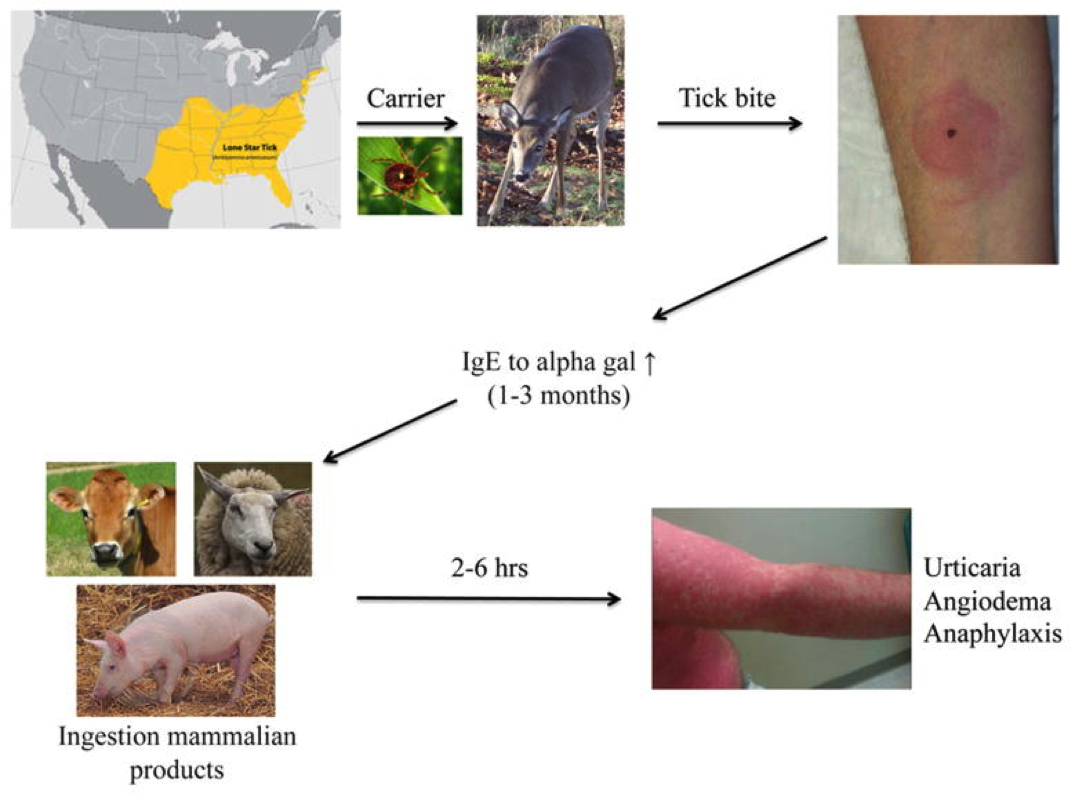
From [5] Steinke, J.W.; Platts-Mills, T.A.E.; Commins, S.P. (2015). The alpha gal story: Lessons learned from connecting the dots. J Allergy Clin Immunol, 135(3): 589-597.
References
[1] Berg, E.A.; Platts-Mills, T.A.E.; Commins, S.P. (2014). Drug allergens and food – the cetuximab and galactose-a-1,3-galactose story. Ann Allergy Asthma Immunol, 112(2): 97-101.
[2] Kroen, G.C. “Ticked Off About a Growing Allergy to Meat.” Science. 16 Nov 2012. Sciencemag.com. <http://www.sciencemag.org/news/2012/11/ticked-about-growing-allergy-meat> 5 June 2017.
[3] McEwen, A.; Kielty, M. (Producer). (2016 October 27). Alpha Gal [Audio podcast]. Retrieved from http://www.radiolab.org/story/alpha-gal/.
[4] Revivicor, Inc. “Xenotransplantation Technology.” 2010. <http://www.revivicor.com/index.html> 5 June 2017.
[5] Steinke, J.W.; Platts-Mills, T.A.E.; Commins, S.P. (2015). The alpha gal story: Lessons learned from connecting the dots. J Allergy Clin Immunol, 135(3): 589-597.






Hiking….for science! What an interesting article. Thanks for sharing.
It never occurred to me that an allergic reaction to red meat can take between 2 and 5 hours to develop after it has been consumed. The other day my friends and I had a guy’s night out and we had steaks and beer for dinner. When I got home, I noticed that I had some hives breaking out. After reading your article, I think I will see a doctor an see if I have an alpha-gal syndrome.