Walter Willett is fifth in the Experience series, after Sara Lawrence-Lightfoot, Martha Minow, Steven Pinker, and E.O. Wilson. Interviews with Melissa Franklin, Stephen Greenblatt, Laurel Thatcher Ulrich, and Helen Vendler will appear in coming weeks.
This article was originally posted in the Harvard Gazette.
For decades, Walter Willett has worked to improve public health by improving diets, most often through research, but sometimes by picking fights: over trans fats, the food pyramid, red meat. Data quality and thick skin have served him well.
Born in 1945 into a Midwestern family with deep ties to farming, Willett did undergraduate study at Michigan State University before getting his M.D. from the University of Michigan. He came to Harvard in the 1970s to continue his medical training and was drawn to the potential for epidemiology to reveal root causes of ailments afflicting his patients, and thereby to prevent them.
The Nurses’ Health Study, an analysis of diet, lifestyle, and health, was an early eye-opener. Willett eventually launched follow-ups, including the Nurses’ Health Study 3 in 2010. His broad outline for healthy living is by now familiar: Don’t smoke, exercise regularly, avoid added sugar and processed foods. He is the Fredrick John Stare Professor of Epidemiology and Nutrition and chair of the Harvard School of Public Health’s Nutrition Department.
Q: I thought we’d start at the beginning. I read that your grandfather was a dairy farmer, is that right?
A: Yes.
Q: But your father was not?
A: He did work in dairy actually. But he was a Ph.D. reproduction physiologist and worked at the American Foundation for the Study of Genetics in the 1950s, when we were living in Madison [Wisconsin]. That meant dairy herd improvement, how to get more milk per cow. So he did research on reproduction biology.
Q: Did you grow up in Madison?
A: We started living on the actual research farm. I started off in a one-room schoolhouse where there was kindergarten through eighth grade in one room. We moved closer to town so I could go to first grade.
Q: You went to Michigan State for undergrad then Michigan for your M.D.; what made you decide to go into medicine?
A: I started off studying physics. We had a close family member who was chair of the Physics Department who got me interested. That was wonderful because it was exact and precise. One of the central aspects of physics is measurement and the study of measurement error, which I have found useful right up to today. [But] I realized that the faculty were mostly working in laboratories in the basement of the physics building, doing seemingly arcane things that felt rather disconnected from the world. I was more interested in seeing the world … so I switched over to food science. [I was] inspired by one faculty member whose course I took, Georg Borgstrom, who was looking at the sustainability of our food supply globally. It got me interested in global issues in food production. Food science was connected with many things of interest to me. I had been a member of the 4-H Club vegetable growers and actually won quite a few blue ribbons at county fairs. Food was interesting. I paid my college tuition at Michigan State growing vegetables. That’s when college tuition was $109 a term, so I didn’t have to make massive profits, but it did keep me interested in food and food production.
Q: Was that a home garden?
A: We lived in a semi-rural area and it turned out the farm next door was owned by someone who was retired. They let me use their land and farming equipment.
Q: How many acres did you farm?
A: It was probably about 3 acres.
Q: All of this happened during your undergraduate years?
A: High school and undergraduate years, but mostly undergraduate. I was interested in the health interface with nutrition and with food science, and decided pretty much at the last minute to go to medical school. I didn’t actually graduate from Michigan State. After three years, I went to the University of Michigan because Michigan State didn’t have a medical school at that time.
Q: Did you eventually get your bachelor’s degree or go right into the medical program?
A: I went right into the medical program. They did allow you to do that.
Q: So you were already interested in nutrition by the time you went to study for your M.D.?
A: Yes. I had [studied] nutrition from different aspects, food production and food science. I have found it useful to have a food science background, because most nutritionists don’t really understand food and food processing and lots of things that go on behind the scenes before it shows up at a grocery store and on a plate. The food science world has been very good in improving the sanitation aspects, the microbial contamination aspects, of food. But, for the most part, processing has otherwise degraded our food supply in an unfortunate way.
Q: Did your interest stem from your family’s involvement in farming?
A: It does come from my family’s involvement in agriculture. My father was interested in biology and, in fact, he did the first ova transplant. That wasn’t done in humans, it was done in dairy cows: fertilized ova transplanted to a different cow. I saw that calf being born in our front yard.
Q: So surrogate parenting started there …
A: Yes, in our front yard. So, there was a strong interest in biology [in my family], and we always had a big home garden. I was in 4-H — that was a family tradition as well — and that got me interested in food, food growing, and production.
Q: At what point did you begin to feel that there were problems with the food supply, with diet? Was that part of this early phase or did that come later?
A: Well, at that time, the general perception was that the problems were more of undernutrition. And that was true, at least on a global basis. We lived in a college community and we always had quite a few foreign students over to our home. Some of them did work in nutrition and they helped get me interested further in nutrition, especially the global aspects of it. During the 1960s, it was thought that protein undernutrition was most important. There was also a general interest in nutrition being a contributing factor to heart disease during that period of time. I took every opportunity to work on nutrition-related research projects during breaks and summers while I was in medical school. I was [also] the subject of nutrition studies. To cut expenses, I found four other classmates and the five of us rented a four-person apartment. We rotated each one of us through the clinical research unit as subjects. So there was always one of us living in the hospital and being the subject of a feeding experiment.
Q: Did you know what the experiment was?
A: It was somewhat mundane in terms of defining dose-response relationships between vitamin C intake and blood level. We had to eat a totally restricted diet for weeks at a time there in the hospital.
One very formative experience was working with a faculty member conducting a small survey in an Indian community in the upper peninsula of Michigan, the Potawatomi tribe. A classmate and I spent a summer up there collecting dietary data, blood measurements, and anthropometric measurements, which was actually very useful to me. We read this paper from [Martha] Trulson and Bertha Burke at the Harvard School of Public Health Department of Nutrition about how to collect dietary data using a food frequency questionnaire. We used that and it turned out to be a very effective way to collect a lot of information about what people were eating. So it did open my eyes to the fact that you could collect dietary data very efficiently. What we learned from structured dietary questionnaires was interesting, but it was also just shocking that about 50 percent of the adults had diabetes. It turns out that this was what was happening to Native American populations across the country. And it raised the obvious question of: “What’s going on? Why do half the adults have diabetes?”
‘You have to develop thick skin, I guess. You can get attacked for things that are just completely untrue.’
Q: Did they know what was going on?
A: No, it was not at all clear. That’s been a background question as our work has unfolded. I think now we understand that much better. It’s clearly related to a susceptibility that isn’t manifested until you have an adverse diet and lifestyle, but also now it’s pretty clear that the foods people were eating were really fuel for diabetes. [The foods] were mainly from the U.S. Department of Agriculture food surplus program, and turn out to be those that will result in high rates of diabetes.
So that was a very formative experience. Then I came to Boston to do an internship and residency in internal medicine at Harvard [Medical] Services at Boston City Hospital. There I met really fantastic faculty members: Ron Arky — Ron was the first attending that I had when I came to Boston; Frank Speizer, who I still work with; Charlie Davidson, who died a couple of years ago and who was very interested in nutrition. So it was quite possible to keep an interest in nutrition alive while I was an intern and resident here, though there wasn’t much occasion for research. One of the other projects I did while I was in medical school was to spend an elective in Tanzania. I really enjoyed that and managed to go back to Tanzania and teach for three years at the University of Dar es Salaam.
I forgot to mention that while I was in residency here, the Vietnam War was going on … I was a conscientious objector and had to do alternative service, which I did working in a health center in East Boston. It was mostly evening clinics, so I could do an M.P.H. here half-time, which was a great experience. It greatly broadened my view of the world and health. [And when I] went to Tanzania, it turned out that they needed people to teach public health there, so I switched from teaching internal medicine to doing that.
Q: So, this was after you graduated from the School of Public Health?
A: Right, yes.
Q: Tell me about Tanzania.
A: Well, that was great. I started off teaching internal medicine, which I enjoyed. With internal medicine here, you largely help people maintain function. But in Tanzania, most people had curable conditions. It was fun to see patients get up and walk away, walk out of the hospital after a few days. But also I appreciated that the bigger challenges, as they are here, were public health issues. So I came to appreciate how much epidemiology could offer. I came back and did a doctoral degree in epidemiology after three years in Tanzania. I was fortunate to work with many great people but especially Brian MacMahon, who was the founder of chronic disease — noncommunicable disease — epidemiology. It offered a perspective we didn’t get in medical school. When someone had a condition like breast cancer, almost never did someone ask why, or if they got cataracts — why? Once you started asking those questions, lots of interesting hypotheses emerged. As it turned out, many of those were related to diet and nutrition. I remember one day, Brian said, “It looks like diet might be an important contributor to breast cancer,” which had never crossed my mind before. At that point in time, very few people were looking at that. Those who were thought that diet might be important in a general way, but it was viewed as too complicated and too difficult to study. It was a relatively untouched area.
Q: Had you begun working on the Nurses’ Health Study by then?
A: Yes. I started when I came back [in the late 1970s]. Frank Speizer was the PI [principal investigator]. I met him as an attending at City Hospital. In the early days, I and one other person ran the Nurses’ Health Study on a day-to-day basis. I did my thesis on smoking and heart disease [using data from] the Nurses’ Health Study. I realized that this could be an ideal setting in which we could study diet in relation to long-term health outcomes, including heart disease and cancer, and other conditions as well. There was a lot of interest in diet and heart disease in the Nutrition Department here. People were being given strong advice on what to eat and what not to eat — for example, to really avoid eggs because they’re high in cholesterol and the cholesterol levels in blood were recognized as one of the most important risk factors for heart disease. Given the strength of the dietary advice, you would have thought there were half a dozen studies showing that people who ate more eggs had higher risk of heart disease, but there were zero such studies. It was a hypothesis, a guess, but there was never any qualification [saying] that it’s our best guess without direct evidence. The recommendation was repeated enough that it became etched in stone. There was one small study on eggs and heart disease from Framingham that showed no relationship, but it was very small. It seemed to me that if we were going to be making recommendations and giving dietary guidance, we needed an empirical basis for doing that, because we could be wrong. The Nurses’ Health Study seemed like it could provide that opportunity. It included a large number, over 100,000 highly motivated participants who could provide high-quality data. And so, in the late ’70s, I worked on pilot testing using standardized questionnaires to collect information on diet. And in 1980, after a series of pilot studies, [we] administered the first dietary questionnaires.
Q: So diet information was not part of the original Nurses’ Health Study?
A: The Nurses’ Health Study was originally narrowly focused on oral contraceptives and breast cancer, with a few added questions on smoking and weight and a few other things. It was a very slim study. In thinking about diet, it was also apparent that we needed to consider physical activity at the same time, and also include questions about alcohol, which were thought to be too sensitive to be asked on the original questionnaire. So we embedded questions on that, along with other beverages. There were a lot of gaps we filled in to give a better picture of the lifestyles of participants.
Q: Have you been at Harvard since then?
A: Yes, I did my doctorate degree when I came back from Tanzania in 1977, then a postdoc and assistant professorship.
Q: How would your career have been different if you had not gotten onto the Nurses’ Health Study?
A: It’s hard to know. The Nurses’ Health Study was intrinsically part of my experience here as a doctoral student. I did continue to do some moonlighting, practicing internal medicine at the East Boston Health Center to support a family while being a student and a postdoc. I could have continued down a primarily clinical pathway, which I enjoyed. But I came to realize that I couldn’t be the kind of internal medicine doctor I wanted to be and also be a leading researcher at the same time. It was certainly beyond my capacity, because both are very demanding.
Q: What was the attraction of research over a clinical career?
A: What I found with clinical internal medicine was that I was seeing so many problems over and over again: congestive heart failure, hypertension, and diabetes. That was somewhat frustrating, because you never cure anyone of these conditions. Certainly, you can help people maintain a better quality of life for a long time, but it seemed to me it would be much better if we could prevent or delay the onset of these conditions.
Q: And where are we in that process now? Clearly we know more.
A: We’ve come a long way in many of these areas. For example, we published in the New England Journal [of Medicine] about 10 years ago an analysis showing that with just moderate diet and lifestyle changes we could prevent about 80 percent of heart disease, and in another paper, 90 percent of type 2 diabetes. So these are largely preventable conditions. For breast cancer, our percentages are lower, but we’ve made some pretty good dents in understanding avoidable causes for breast cancer. For colorectal cancer, quite a large fraction can be prevented by diet and lifestyle. So we’ve come a long way and life expectancy has increased quite a bit since the 1960s. The rates of heart disease and cardiovascular mortality have fallen over 60 percent since that time. But there’s still a huge gap between what we know and what actually is being put into practice. In the same paper that showed that heart disease is about 80 percent preventable, only about 4 percent of the participants in the Nurses’ Health Study were practicing all the elements of a healthy lifestyle. So there are huge gaps between the potential for prevention and reality, and growing gaps by economic and racial divisions in this country. Part of the population, those with more education and resources, has been very efficiently taking up this information and incorporating it into their lives, but other parts of the population have had minimal changes. In some groups, life expectancy has gone down for complex reasons related to education and poverty. So we’ve made huge progress in understanding. We’ve made, on average, considerable progress in improving diets and lifestyle, but there’s still a lot to learn and even more to do in terms of implementation.
Q: So we have a good idea of the important steps to take, but we have these enormous obesity and diabetes epidemics under way. Is our health, as it relates to nutrition, better now than it was in the ’70s?
A: Yes it is, on average, but the average hides massive variability. Our nutrition is better and we’ve benefited from that [in terms] of life expectancy. Back in the ’50s and ’60s, it was almost routine that men had a massive MI [myocardial infarction, or heart attack] in their 50s and often died from it. It was the big one that people expected at age 55. That kind of event happens rarely now.
Q: Your work has touched so many different areas, hundreds and hundreds of papers, is there a particular one that, when you think back on your career, was the best, or most important, or most enduring?
A: Probably some of the most important papers were not ones that got the most attention. They were more methodologically oriented, showing that, yes, we can measure diet in large populations using the techniques we’ve used in the Nurses’ Health Study, which became the foundation for a lot of other work. But in terms of more substantive topics, probably the work on trans fats has been the most interesting and satisfying and has gone though the implementation cycle now pretty well. I was interested in trans fats from the time we started the dietary assessment work in the ’70s. At that time, [there was] laboratory work documenting the importance of prostaglandins [a kind of fat molecule] in many physiological processes. What I realized, partly from my food science background, is that we were taking natural vegetable oils — corn oils and soybean oils — and partially hydrogenating them. These oils were mostly made up of essential fatty acids that were the precursors of the prostaglandins and we were twisting the shape of these molecules. That seemed like a really risky thing to be doing. When you change the shape of those essential molecules, they will not have the same function. It was quite unpredictable what that would do, but it’s unlikely when you throw sand in a finely working Swiss watch, that it will work better.
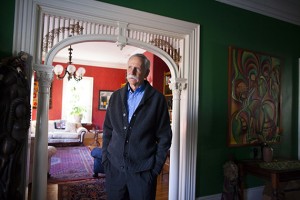
Data collected over the past few decades should soon start to yield more insights on mental and cognitive function, said Willett, pictured at his Cambridge home.
Q: You called attention to that. It has worked through the regulatory process and recently the government took action.
A: Trans fats had been in the category called GRAS, or generally recognized as safe. And the FDA has recently said that the evidence no longer supports the conclusion that trans fats are generally recognized as safe. They could have said that 15 years ago, but they finally said it. And there’s a 60-day comment period, but no one would dare say they’re generally recognized as safe today. That means they can’t be added to foods without special approval, which will effectively eliminate trans fat in our food supply. That was quite a long process because we had to create a database — no one had a comprehensive database of the trans fat content of commonly eaten foods in the United States. There had been some measurements made, but it was haphazard as to what was measured. We obtained data from different laboratories and also set up an analysis system so we could measure trans fats in foods and continually update the analyses. It was a lot of work, because the manufacturing process was changing over time and if we didn’t keep updating that information we would have missed what was happening.
So this was a big effort by many people in our group over 30 years and our findings turned out to be extremely controversial. The main heart disease prevention establishment had pretty much decided that saturated fat was the problem. They really attacked us for raising this distraction, that trans fat might be a problem, as did the food industry for different reasons. We were very much by ourselves out on a limb for quite a while. But we kept accumulating data. And other people looked at this and virtually everyone found that trans fat was a problem.
Q: You’re clearly no stranger to controversy. Do you have any advice to students and young researchers coming up for when they get a result that they think might be unpopular?
A: Well, there’s no question that having the best and strongest data is most fundamentally important. That is the good thing about science: There is a process of replication and improvement of data quality. And sometimes it’s not at all a straight line process, but doing everything possible to have the best data possible is certainly the first thing to do. I think that there has been a debate within science, at least within epidemiology, whether scientists should be engaged in discussions about the interpretation of results and policy. Some say, “No, just publish the data, your responsibility ends there: Somebody else should interpret the data. Leave that to the policymakers.” But I think if that’s what I had done, our findings would have just been buried. Policymakers, most of them, don’t understand the issues nearly as well as the people working with the data. And there were powerful interests, both from the well-intended cardiovascular prevention community and also the economically influenced manufacturing industry, that really wanted to have these results ignored or dismissed. So I think at certain times, and with care and caution to be as objective as possible, it is appropriate to be part of that discussion and not let potentially important findings be buried.
Q: What about the personal challenge of managing controversy? Do you need to take a deep breath when you know the fight is coming? Do you ever think, “Geez, this may not be worth it?”
A: Well, yeah, you have to develop thick skin, I guess. You can get attacked for things that are just completely untrue. One of the whisper campaigns [was that] I was bought out by the olive oil industry — when I never got a penny from the olive oil industry — and things like that. So you do have to have thick skin. And it’s important to recognize it’s possible that your data are wrong. Every study has the possibility of getting a wrong answer for many different reasons and that’s why it is really important that there be confirmatory evidence. And then it also does depend on whether it’s something that’s important enough to be worth a fight. But in this case it was. We calculated that the number of deaths per year potentially due to trans fat in the diet were running in the tens of thousands. That’s not trivial and it was worth spending the extra effort, not allowing this to get buried, which would have been most convenient for many parties.
Q: How about missteps along the way? Have there been mistakes you regretted? How do you handle that sort of thing and how do you recover from it?
A: We had a couple of events that fortunately didn’t make a big difference in the long run. We did have [one] when we were launching the Health Professionals Follow-up Study, our cohort of men. It almost crashed at the beginning because of a programming error — made by someone no longer here — that resulted in each ID number being sent to 10 different people. Of course, we take great effort to have questionnaires come back to us [without] names and addresses to maintain confidentiality. We realized pretty quickly when we started getting mail returns that we were in deep trouble. Fortunately, many people did send back their questionnaire with a name and address on the envelope. If that was true we could right away identify the person. But not everybody did, so we spent two years and many resources sorting that out. We eventually had to exclude several hundred people, which wasn’t too bad out of 50,000. So we have had technical issues like that, even though we have quite a bit of quality control, redundancy, and safety checks. Basically, I believe in Murphy’s Law, that if something can go wrong, it will go wrong, as a very fundamental principle, and I spend a fair amount of time thinking about what might go wrong. Still, to this day, new issues arise that we didn’t anticipate. There’s almost never too much quality control and redundancy in big studies like this where so much is at stake.
We just had a paper in BMJ [in which] there was one variable that was misinterpreted slightly by one person in our group and almost every number in the manuscript was off by a slight amount. It was something that didn’t change any conclusions, but we still had to correct it. I think we have never had … of the thousands of papers we published, an error that changed conclusions, but we’ve had a few small errors that we wish we’d avoided, and work hard to prevent those.
Q: What advice do you have for a young researcher starting out today?
A: I found it tremendously useful to have had experiences from a wide variety of fields that may sometimes seem disconnected. However, that’s where the interesting new connections often arise and how we can bring a different perspective to an unsolved problem. This may not work for every field, but at least for [those going into] public health, I would encourage a young researcher to take every opportunity to see the world from a different perspective. That may turn out to be very useful in an unpredictable way, and if not, it will have made your life more interesting. Obviously, we need to dig down deeply into our research topic, but too often we’re only told to focus, focus, focus. Finding the right balance between focusing and having a broad perspective is critical.
Q: What, to your mind, is most exciting in public health today?
A: I think one of the big frontiers is the mind and the central nervous system. We know less about that than about other organ systems and relatively little about the causes of Alzheimer’s disease and Parkinson’s disease, so we’re putting more emphasis on that. The timing is good. When we started and our participants were relatively young, there was almost none of that [Alzheimer’s and Parkinson’s] in our cohort. Now, with three or four decades of data, people are developing these kinds of conditions, so we can connect what people were doing 30 and 40 years ago with their mental function and cognitive function.
The whole area of the microbiome is very interesting. For decades, we thought the fecal microbiome was really important, but didn’t really have the tools to study it. We did some pilot work back in the early ’80s and our dietitian said, “If you do one more stool collection like that, I’m quitting.” We had to have fresh feces, with viable organisms. Now, by analyzing the genes, you don’t have to have the living bacteria.
It [also] goes back to what got me interested in nutrition in the first place. On a global basis, there are huge issues about being able to feed the world’s population a healthy diet in a sustainable way. This is a major issue and it goes back to the farm and the way we’re producing food now. We still have our family farm in Michigan, run by an uncle, but it is unrecognizable now. It was small fields and hedgerows, just teeming with biodiversity. It’s all [been] flattened into massive fields of corn, of soybean, which is what has happened across our country. When we look at the grain produced in the United States, only about 10 percent is eaten by Americans. Most is fed to animals and converted to ethanol for fuel.
I’ve seen the world change before my eyes. We have a little place in New Hampshire. A little island called Toad Island because there were toads all over the island when we bought it in the 1970s. This last summer, there were zero toads. And we went to a little field where there’s milkweed and there’s always lots of monarch butterflies — there were no monarchs this year. And, of course, the honeybee population is precarious. There’s obviously multiple factors operating here, but we are destroying the biome’s diversity very rapidly. The fact that extinction is happening right before my eyes is amazing and profoundly disturbing. So, somehow, we have to have some constraints and some limits to the way we are dealing with our environment to maintain biodiversity and, in the end, produce healthy food in a sustainable way. That will be a very big issue in the coming decades.





Leave a Reply